All content on this site is intended for healthcare professionals only. By acknowledging this message and accessing the information on this website you are confirming that you are a healthcare professional. If you are a patient or carer, please visit the International Myeloma Foundation or HealthTree for Multiple Myeloma.
The Multiple Myeloma Hub website uses a third-party service provided by Google that dynamically translates web content. Translations are machine generated, so may not be an exact or complete translation, and the Multiple Myeloma Hub cannot guarantee the accuracy of translated content. The Multiple Myeloma Hub and its employees will not be liable for any direct, indirect, or consequential damages (even if foreseeable) resulting from use of the Google Translate feature. For further support with Google Translate, visit Google Translate Help.
The Multiple Myeloma Hub is an independent medical education platform, sponsored by Bristol Myers Squibb, GSK, Legend Biotech, Pfizer, and Roche. Funders are allowed no direct influence on our content. The levels of sponsorship listed are reflective of the amount of funding given. View funders.
Now you can support HCPs in making informed decisions for their patients
Your contribution helps us continuously deliver expertly curated content to HCPs worldwide. You will also have the opportunity to make a content suggestion for consideration and receive updates on the impact contributions are making to our content.
Find out more
Create an account and access these new features:
Bookmark content to read later
Select your specific areas of interest
View multiple myeloma content recommended for you
Defining relapsed and refractory MM: the challenges and controversies
Do you know... The definition of a clinical relapse includes multiple criteria. Which of the following options is included in the International Myeloma Working Group (IMWG) criteria for a clinical relapse?
Patients with relapsed/refractory multiple myeloma (RRMM) are a diverse group. Three distinct subgroups can be identified within this category:
-
Patients who relapsed while not on active treatment
-
Patients who relapsed while on active treatment and became refractory
-
Patients with primary refractory MM
In addition, RRMM can refer to patients who relapse early after first-line treatment, as well as to patients who relapse after several lines of therapy or after a long duration of remission. This makes patients with RRMM a very heterogeneous group to treat. Furthermore, new therapies added to the treatment armamentarium in recent years increases the complexity of selecting and sequencing treatments for each patient.1
In clinical trials, it is important to have a homogenous group of patients, which in turn requires clear definitions to be used in the selection criteria of what constitutes a patient experiencing a relapse or becoming refractory to a specific agent. Some studies can use vague terms such as “exposure”, which does not specify the dose or duration of treatment. This can lead to enrollment of a mixed patient population and the need for subgroup analyses, making the interpretation of results and their application into practice more difficult. These definitions are also important for drug approvals to accurately identify the population that can be treated with a specific agent.1
Defining relapsed and refractory MM
The International Myeloma Working Group (IMWG), European Hematology Association (EHA) and European Society for Medical Oncology (ESMO), American Society of Hematology, and the U.S. Food and Drug Administration (FDA) Workshop reached a consensus on certain key definitions, a summary of which can be found in Figure 1.
Figure 1. Key definitions in multiple myeloma
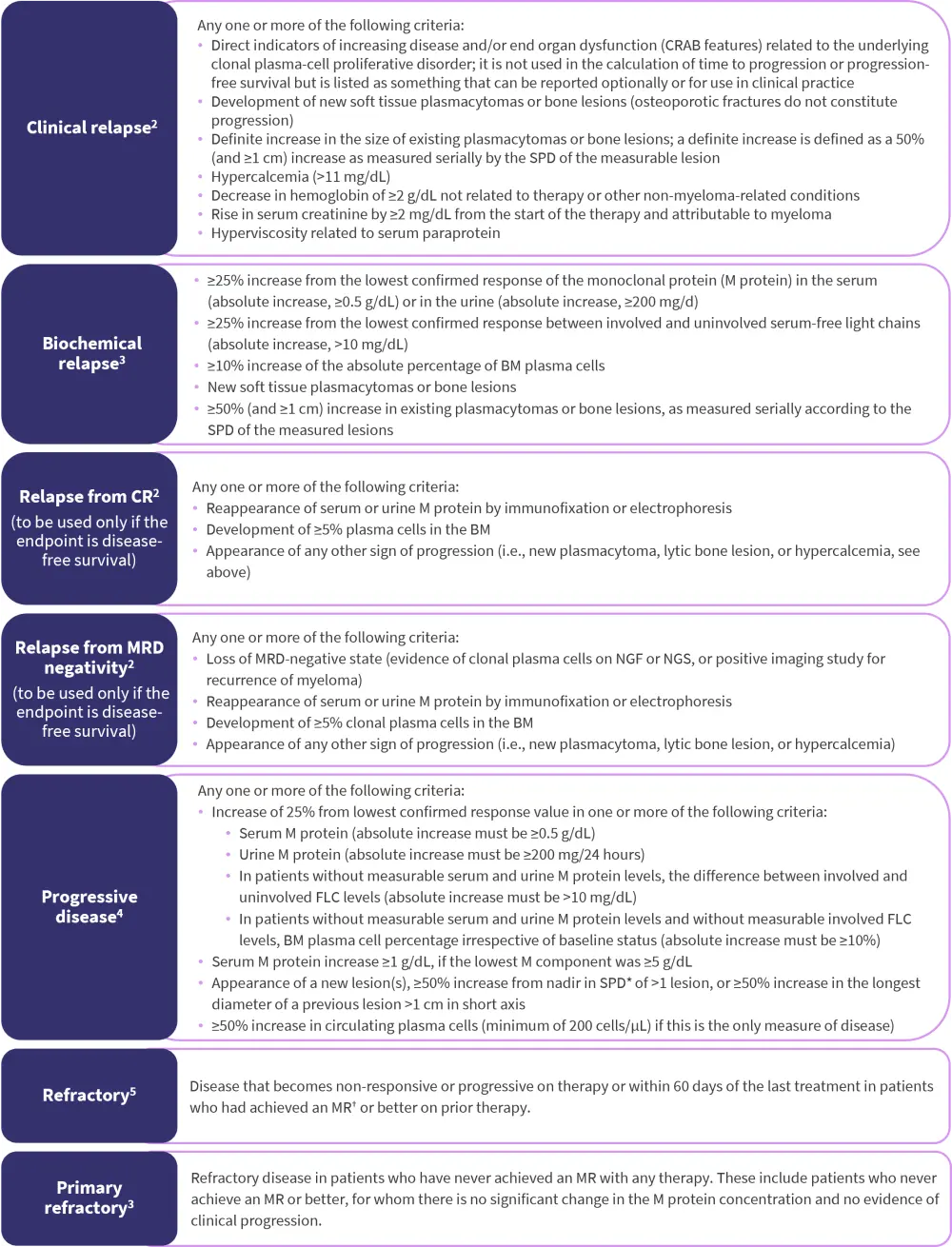
BM, bone marrow; CRAB, calcium, renal, anemia, bone disease; FLC, free light chain; MR, minimal response; MRD, measurable residual disease; NGF, next-generation flow; NGS, next-generation sequencing; SPD, sum of the products of the maximal perpendicular diameters of measured lesions.
*Plasmacytoma measurements should be taken from the CT portion of the PET/CT, or MRI scans, or dedicated CT scans where applicable. For patients with only skin involvement, skin lesions should be measured with a ruler. Measurement of tumor size will be determined by the SPD.
†MR: ≥25% but ≤49% reduction of serum M protein and reduction in 24-hour urine M protein by 50–89%. In addition to the above listed criteria, if present at baseline, a ≥50% reduction in the size (SPD†) of soft tissue plasmacytomas is also required.
Current challenges with the definitions in clinical research
A number of clinical trials use the inclusion criteria of progressive disease rather than clinical relapse, which encompasses patients showing signs of early biological/biochemical progression, as well as patients in clinical relapse (Figure 1). These two groups may have very different prognoses and outcomes; thus, trial results may depend on the proportion of patients in each group in addition to the treatment intervention being examined.6
Not all clinical trials use clear definitions; for example, as shown in Table 1, patients in which ≥3 lines of therapy “failed” are included in the DREAMM-2 trial.7 This could encompass patients who are intolerant to treatment due to adverse events, who have relapsed on treatment/become refractory, or who have discontinued due to non-compliance.
Table 1. Examples of clinical trial variability in definitions for relapsed/refractory MM in inclusion criteria
|
IMiD, immunomodulatory drug; IMWG, International Myeloma Working Group; mAb, monoclonal antibody; MM, multiple myeloma; PI, proteasome inhibitor; PR, partial response. |
|||
|
NCT number |
Treatments investigated |
Inclusion criteria/ |
|
|---|---|---|---|
|
Trials selecting patients with relapsed and double-refractory MM |
|||
|
ICARIA-MM8 |
Isatuximab, pomalidomide, and dexamethasone versus pomalidomide and dexamethasone |
Participants had “failed” treatment with lenalidomide and a PI (bortezomib, carfilzomib, or ixazomib) alone or in combination (intolerant or progression within 6 months after reaching PR or better). |
|
|
APOLLO7 |
Daratumumab, pomalidomide, and low-dose dexamethasone versus pomalidomide and low-dose dexamethasone |
Subjects must have received prior antimyeloma treatment, which must have included both PI- and lenalidomide-containing regimens. The subject must have had a response (i.e., PR or better based on the investigator's determination of response as defined by the modified IMWG criteria) to prior therapy. |
|
|
Trials selecting patients with relapsed and triple-refractory MM |
|||
|
STORM9
|
Selinexor and dexamethasone |
Refractory to previous treatment with one or more glucocorticoids, parenteral PI (i.e., bortezomib and/or carfilzomib), IMiD (i.e., lenalidomide and/or pomalidomide), and the anti-CD38 mAb, daratumumab. Refractory is defined as ≤25% response to therapy, or progression during therapy or within 60 days after completion of therapy. |
|
|
DREAMM-210 |
Belantamab mafodotin |
Participants with a histologically or cytologically confirmed diagnosis of MM as defined in the IMWG 2014 criteria, had undergone a stem cell transplant or were considered transplant ineligible, had “failed” ≥3 prior lines of antimyeloma treatments, including an anti-CD38 antibody (e.g., daratumumab) alone or in combination, and was refractory to an immunomodulatory drug (i.e., lenalidomide or pomalidomide) and to a proteasome inhibitor (e.g., bortezomib, ixazomib, or carfilzomib). |
|
A similar problem occurs with definitions of the term “refractory” especially when a patient is refractory to more than one agent. With the advent of so many novel agents, the different combinations can be numerous, and patients must be defined as refractory to a specific agent, not double refractory alone. Looking at the literature, multiple definitions can be found for double refractory, ranging from “MM that is relapsed and/or refractory to bortezomib and lenalidomide”11 to “MM refractory to both proteasome inhibitors and immunomodulatory agents”12.
Conclusion
While the IMWG and EHA-ESMO guidelines have advanced how we categorize patients with RRMM, further work in standardization needs to be done. Refractoriness definitions naturally evolve with the changes in standard of care and the approval of new agents, but still, care must be taken when comparing patient groups between trials as this shows that double or even triple refractory patients may have different definitions between studies. Ongoing trials in advanced disease show that this field will gain more and more layers of complexity since the selection criteria now include definitions for quad- and penta-refractory MM. Inclusion criteria need to be specific to ensure a homogenous group of patients; however, some consensus is urgently needed, for example, to narrow down whether patients in biochemical relapse should be included along with those in clinical relapse under the heading of progressive disease.
References
Please indicate your level of agreement with the following statements:
The content was clear and easy to understand
The content addressed the learning objectives
The content was relevant to my practice
I will change my clinical practice as a result of this content




