All content on this site is intended for healthcare professionals only. By acknowledging this message and accessing the information on this website you are confirming that you are a healthcare professional. If you are a patient or carer, please visit the International Myeloma Foundation or HealthTree for Multiple Myeloma.
The Multiple Myeloma Hub website uses a third-party service provided by Google that dynamically translates web content. Translations are machine generated, so may not be an exact or complete translation, and the Multiple Myeloma Hub cannot guarantee the accuracy of translated content. The Multiple Myeloma Hub and its employees will not be liable for any direct, indirect, or consequential damages (even if foreseeable) resulting from use of the Google Translate feature. For further support with Google Translate, visit Google Translate Help.
The Multiple Myeloma Hub is an independent medical education platform, sponsored by Bristol Myers Squibb, GSK, Legend Biotech, Pfizer, and Roche. Funders are allowed no direct influence on our content. The levels of sponsorship listed are reflective of the amount of funding given. View funders.
Now you can support HCPs in making informed decisions for their patients
Your contribution helps us continuously deliver expertly curated content to HCPs worldwide. You will also have the opportunity to make a content suggestion for consideration and receive updates on the impact contributions are making to our content.
Find out more
Create an account and access these new features:
Bookmark content to read later
Select your specific areas of interest
View multiple myeloma content recommended for you
Opportunistic infections in multiple myeloma part I: Etiology and incidence
Opportunistic infections (OI) are infections that occur more frequently or more severely in individuals with a compromised immune response. Patients with multiple myeloma (MM) are at a significantly higher risk of contracting OI, estimated at seven times higher than in the general population.1 In addition to a higher risk, patients with MM are also at an increased risk of poorer outcomes as a result; with 45% of early deaths attributable to infections.1
Specific infections, such as pneumonia and septicemia, have been found to be at an even higher risk for patients with MM, at ten times higher than the general population in the first year after diagnosis.1
Figure 1. Fast facts on the risk of infection in patients with MM*
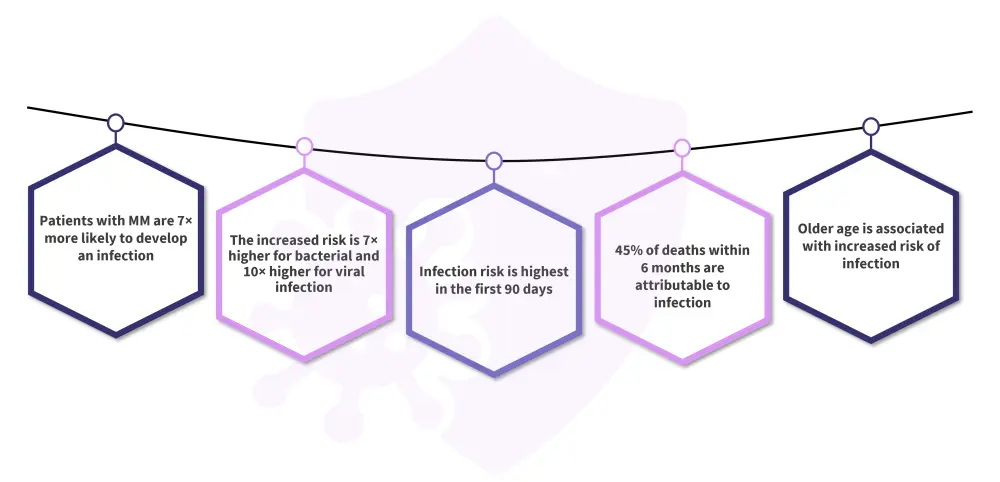
MM, multiple myeloma.
*Data from Blimark, et al.1 and Allegra, et al.2
Secondary immunodeficiency in MM
Immunodeficiency in MM is characterized by the inability to eliminate pathogens and tumor cells. Secondary immunodeficiency in patients with MM is attributable to the principal disease; but is also a common effect of MM therapies.
Principal disease2
A key characteristic of MM is the abnormal proliferation of clonal plasma cells. This abnormality leads to an excess production of a single damaged immunoglobulin and of light chain antibodies, which cannot incite an effective immune response. MM plasma cells are responsible for inhibiting polyclonal B lymphocytes, resulting in hypogammaglobulinemia. Neoplasia of MM plasma cells results in reduced normal cell proliferation (Figure 2).
Figure 2. Mechanisms of immunodeficiency in MM*
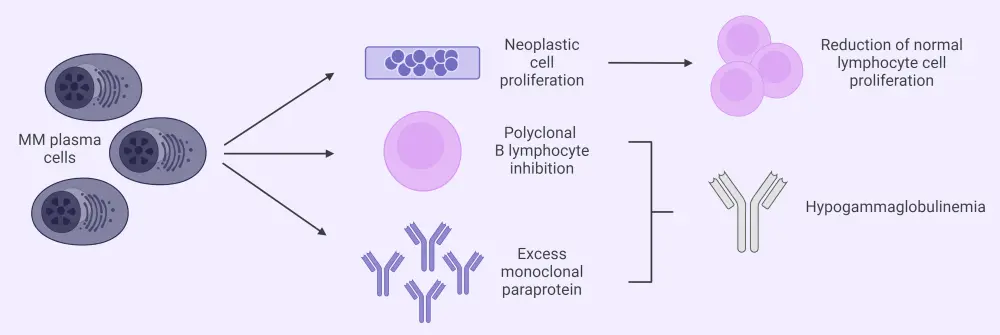
CAR, chimeric antigen receptor; MM, multiple myeloma.
*Adapted from Allegra, et al.2
Treatment-related immunodeficiency
Immunomodulatory agents (IMiD)3,4
IMiD, such as lenalidomide and pomalidomide, are commonly used in combination at all stages of MM treatment, and as a maintenance therapy after autologous stem cell transplantation. Neutropenia, myelosuppression, thrombocytopenia, and serious infection are all associated with the use of IMiD.
Relative risk of infection with IMiD therapies:
- Overall incidence of serious infection, 11.6%
- Rates of serious infection on induction, maintenance, and in relapsed/refractory MM, 12.3%, 8.2%, and 7.2%, respectively
- Incidence of Grade ≥3 neutropenia, 41.5%
- Relative risk for IMiD compared with non-IMiD therapies, 2.59 (p < 0.01)
Overall, patients with relapsed/refractory MM treated with pomalidomide-based regiments are at the highest risk of infection, observed at 23%. However, IMiD induction in patients eligible for autologous stem cell transplantation has also been found to decrease the risk of serious infection at a relative risk of 0.82.5
Proteasome inhibitors4
Proteasome inhibitors (PI), such as bortezomib, have been found to be associated with MM cell apoptosis and T-cell immunosuppression.
Relative risk of infection with PI-based therapies:
- Rate of severe infection with PI-based induction in patients ineligible for transplant (19.7%)
- Bortezomib-based induction therapy is associated with a two-fold risk increase of severe infection than thalidomide IMiD therapy
Alkylating agents5
Alkylating agents, such as cyclophosphamide, have immunosuppressive and immunomodulatory properties. Cyclophosphamide causes apoptosis by forming cross-links and damaging DNA, leading to neutropenia, thrombocytopenia, and anemia.7
Monoclonal antibodies (mAbs)6
mAbs target specific antigens to elicit a therapeutic effect. However, they also reduce effector cell function and deplete T- and B-cell lymphocytes, leading to immunosuppression. The increased risk of infection associated with mAbs is particularly evident with anti-CD38 antibody treatment.
Relative risk of infection with anti-CD38 antibody therapy:
- Incidence of any-grade infections, 77%
- Incidence of severe infection, 28%
- Increased risk of pneumonia, 39%
- Increased risk of severe pneumonia, 38%
Bispecific antibodies7
Both hypogammaglobulinemia and an increased risk of infections have been observed with bispecific antibody (bsAb) therapies. Of note, bsAb which targets B-cell maturation antigen (BCMA) have been recorded to further increase this risk, compared with other targets, such as G-protein coupled receptor family C group 5 member D (GPRC5D) and Fc Receptor-Like 5 (FcRH5).
Relative risk of infection with bsAb therapy:
- Incidence of infection, 50%
- Any-grade neutropenia, 38.6%
- Hypogammaglobulinemia, 75.3%
- Deaths associated with bsAb-related infection, 25.5%
- Non-BCMA-targeted bsAb resulted in a lower incidence of infection than BCMA-targeted bsAb:
- Grade 3/4 neutropenia, 25.3% and 39.2%, respectively
- Grade 3/4 infections, 11.9% and 30%, respectively
Chimeric antigen receptor (CAR) T-cell therapies8
Multiple factors contribute to the increased immunosuppression with CAR T-cell therapy, including prior cytotoxic and lymphocyte-depleting therapies. Infections are commonly observed in patients post CAR T-cell infusion; and are a cause of increased morbidity and mortality rates.
Relative risk of infection with BCMA-targeted CAR T-cell therapies:
- Infection rate at a median follow-up of 6 months, 53%
- 50% occurred within the first 100 days after infusion
- Bacterial, viral, and fungal infections, 40%, 53%, and 6%, respectively
- Grade 3/4 neutropenia at ≤1 month, 98%
- Hypogammaglobulinemia at 1-year post infusion, 76%
Figure 3. Summary of the contributing elements to secondary immunodeficiency in MM*
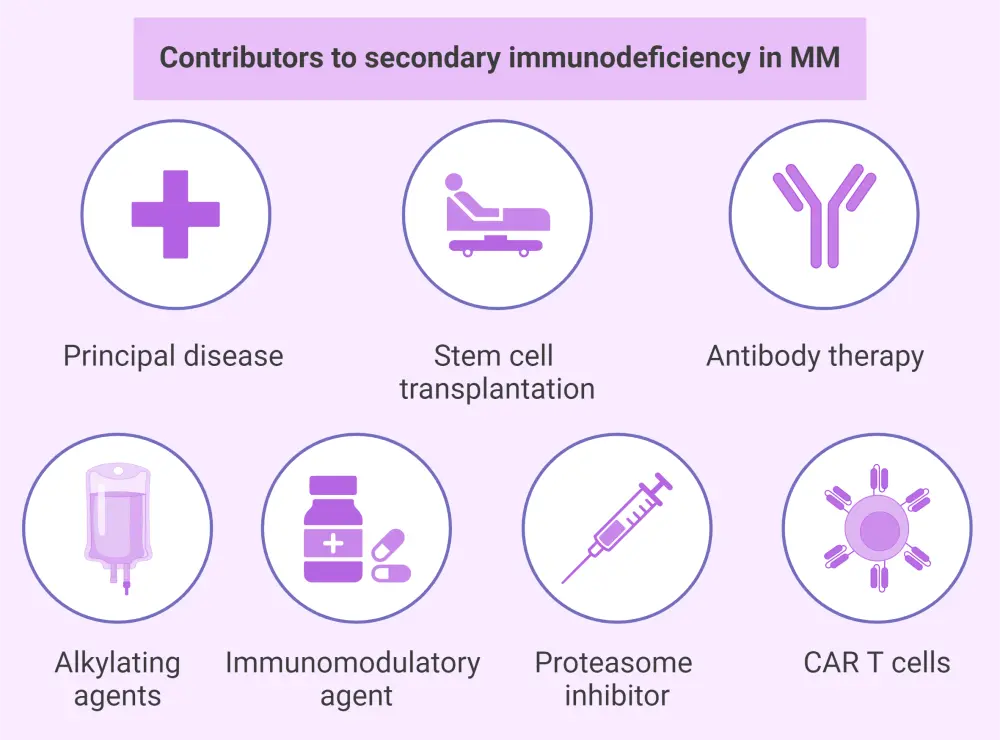
CAR, chimeric antigen receptor; IMiD, immunomodulatory agent; MM, multiple myeloma; PI, proteasome inhibitor.
*Data from Blimark, et al.1 and Allegra, et al.2 Created with BioRender.com.
Conclusion
Patients with MM are an at risk group for OI and are associated with increased mortality rates. Both MM itself and MM therapies contribute to immunodeficiency. This consistently increased risk, particularly in the heavily pretreated population, highlights the need for effective management and prophylaxis which has been covered by the Multiple Myeloma Hub in part II of this article series.
References
Please indicate your level of agreement with the following statements:
The content was clear and easy to understand
The content addressed the learning objectives
The content was relevant to my practice
I will change my clinical practice as a result of this content

