All content on this site is intended for healthcare professionals only. By acknowledging this message and accessing the information on this website you are confirming that you are a healthcare professional. If you are a patient or carer, please visit the International Myeloma Foundation or HealthTree for Multiple Myeloma.
The Multiple Myeloma Hub website uses a third-party service provided by Google that dynamically translates web content. Translations are machine generated, so may not be an exact or complete translation, and the Multiple Myeloma Hub cannot guarantee the accuracy of translated content. The Multiple Myeloma Hub and its employees will not be liable for any direct, indirect, or consequential damages (even if foreseeable) resulting from use of the Google Translate feature. For further support with Google Translate, visit Google Translate Help.
The Multiple Myeloma Hub is an independent medical education platform, sponsored by Bristol Myers Squibb, GSK, Legend Biotech, Pfizer, and Roche. Funders are allowed no direct influence on our content. The levels of sponsorship listed are reflective of the amount of funding given. View funders.
Now you can support HCPs in making informed decisions for their patients
Your contribution helps us continuously deliver expertly curated content to HCPs worldwide. You will also have the opportunity to make a content suggestion for consideration and receive updates on the impact contributions are making to our content.
Find out more
Create an account and access these new features:
Bookmark content to read later
Select your specific areas of interest
View multiple myeloma content recommended for you
Patient outcomes in MM: Global disparities
Do you know... Which factor was NOT attributable to poorer clinical outcomes in any country except for the United States (U.S.)?
The treatment of multiple myeloma (MM) has improved over time, with more standardized therapies becoming available globally. However, significant differences exist in the incidence of MM, access to novel therapies and transplant, and survival outcomes. The primary factors attributable to these discrepancies include age, sex, ethnicity, socioeconomic status, and geographical location.1
Here, we summarize the discrepancies between the management of MM globally, with a focus on the differences between and within international regions.
Regional disparities in MM
Socioeconomic status and its impact on treatment can be observed at a large scale between the margins of global wealth. However, this disparity can also be seen within small geographic regions, where discrepancies in resources are comparatively smaller but still influence both the likelihood of seeking and access to treatment. Other factors, such as age, do not differ significantly between countries but are consistently related to poorer access and survival, regardless of location.1
A summary of the incidence and disparity in treatment for MM is shown by geographical region in Figures 1, 2 and 3.
Figure 1. Disparities in MM incidence and treatment in the Americas*
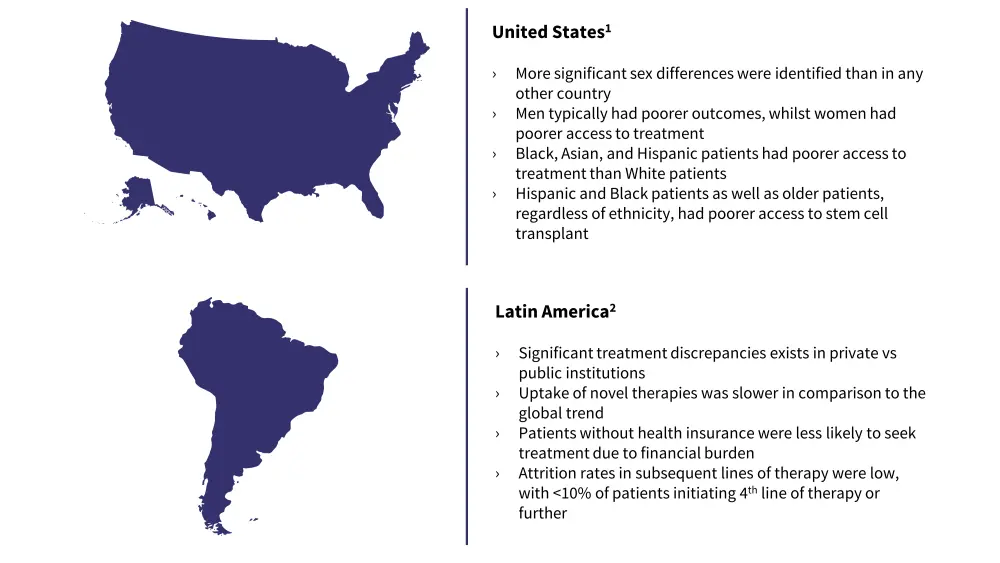
*Data from Mateos, et al.1and Hungria.2
Figure 2. MM Incidence and treatment in Asia*

HSCT, hematopoietic stem cell transplantation.
*Data from Ganguly, et al.3 and Tan, et al.4
Figure 3. MM incidence and treatment in Europe*
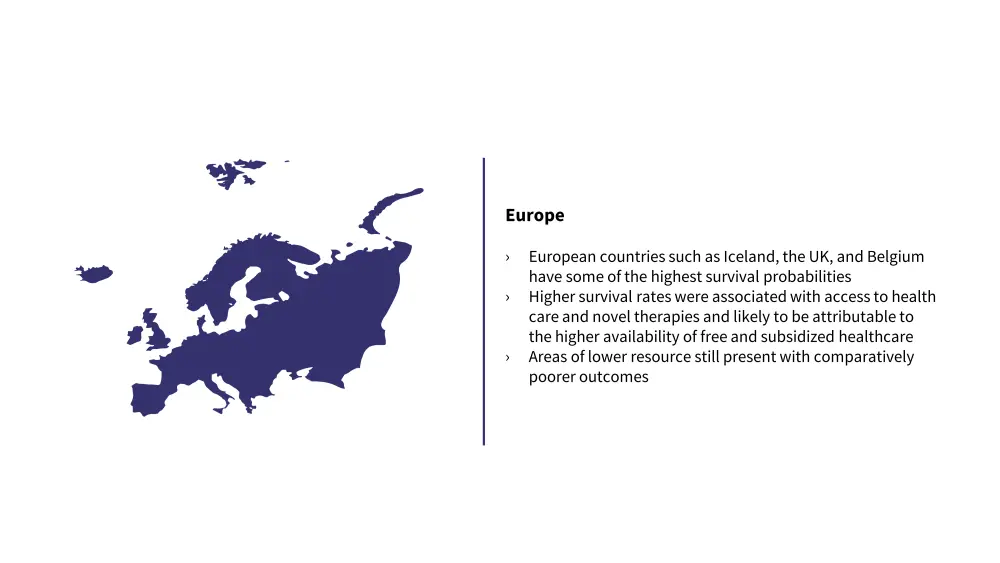
*Data from Ludwig, et al.5
Global disparities in MM
Globally, factors consistently related to improved outcomes in MM included access to novel therapies, private treatment facilities, socioeconomic status, and younger age.1 Disparities between regions were more difficult to establish, with the most significant differences noted within countries or smaller communities. New Zealand and select European countries presented with the highest overall likelihood of survival, but internal analysis also revealed a spectrum of healthcare quality comparable to countries with a lower likelihood of survival.5 A snapshot of the global differences in myeloma treatment are shown in Figure 4.
Figure 4. Global disparities in MM treatment*
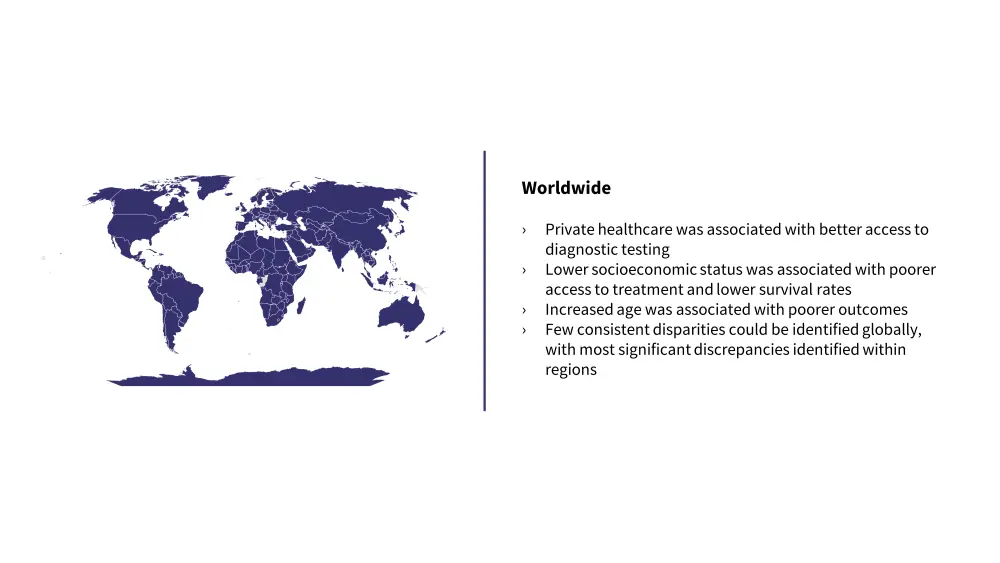
*Data from Mateos, et al.1
Conclusion
The challenges to healthcare equality in MM management vary by geographical regions. However, a few recurring factors present as consistent determinants of poor outcomes including, older age, and socioeconomic status. Whilst these factors are common worldwide, their influences are most prevalent when examined within each region.
Sufficient research from which to draw clear conclusions regarding global MM is lacking. However, existing research has identified specific populations and factors for further research and areas on which outreach effort should be focused, notably in populations with lower socioeconomic status and older age.
Expert Opinion
“In Latin American countries, approximately 88% of the multiple myeloma patients receive treatment from the public healthcare system. Access to exams, ranging from simple diagnostics to molecular testing, is very limited. Few patients have access to cytogenetic tests. Studies show that the majority of the patients present advanced-stage disease at diagnosis. Access to novel therapies is usually very limited, due to delayed approval or incorporation, mainly in public institutions. Transplant availability is also limited, and there is a great disparity in outcomes and survival between public and private healthcare facilities. The main challenge in Latin America is the incorporation of the novel agents in the treatment of all of the MM patients and, thus, to reach the same outcome in survival in both public and private settings.”
 Vania Tietsche de Moraes Hungria
Vania Tietsche de Moraes HungriaExpert Opinion
"Disparities continue to exist in outcomes for patients with multiple myeloma (MM). In this manuscript recently published, we performed a rapid evidence assessment to evaluate the effect of an array of sociodemographic factors such as age, sex, race/ethnicity, socioeconomic status, and geographic location on diagnosis, access to treatment, and patient outcomes. We searched for observational, real-world articles and found that increasing age and low socioeconomic status were consistently associated with worse patient outcomes worldwide. In the USA, men typically had worse outcomes than women, although women had poorer access to treatment. Our study highlights specific patient populations with MM that remain at a disadvantage and for whom there is potential scope for improvement in outcomes. Acknowledging and addressing the causes and effects of disparities in patient outcomes may help to develop novel treatments or treatment strategies for MM, for instance through the enrolment of more diverse and representative patient populations in clinical trials, and to improve access to treatment and treatment facilities in the real world."
 María-Victoria Mateos
María-Victoria MateosReferences
Please indicate your level of agreement with the following statements:
The content was clear and easy to understand
The content addressed the learning objectives
The content was relevant to my practice
I will change my clinical practice as a result of this content

