All content on this site is intended for healthcare professionals only. By acknowledging this message and accessing the information on this website you are confirming that you are a healthcare professional. If you are a patient or carer, please visit the International Myeloma Foundation or HealthTree for Multiple Myeloma.
The Multiple Myeloma Hub website uses a third-party service provided by Google that dynamically translates web content. Translations are machine generated, so may not be an exact or complete translation, and the Multiple Myeloma Hub cannot guarantee the accuracy of translated content. The Multiple Myeloma Hub and its employees will not be liable for any direct, indirect, or consequential damages (even if foreseeable) resulting from use of the Google Translate feature. For further support with Google Translate, visit Google Translate Help.
The Multiple Myeloma Hub is an independent medical education platform, sponsored by Bristol Myers Squibb, GSK, Legend Biotech, Pfizer, and Roche. Funders are allowed no direct influence on our content. The levels of sponsorship listed are reflective of the amount of funding given. View funders.
Now you can support HCPs in making informed decisions for their patients
Your contribution helps us continuously deliver expertly curated content to HCPs worldwide. You will also have the opportunity to make a content suggestion for consideration and receive updates on the impact contributions are making to our content.
Find out more
Create an account and access these new features:
Bookmark content to read later
Select your specific areas of interest
View multiple myeloma content recommended for you
Cilta-cel for relapsed/refractory MM: updated results from the CARTITUDE-1 and CARTITUDE-2 trials
Featured:
Ciltacabtagene autoleucel (cilta-cel) is a B-cell maturation antigen-directed autologous chimeric antigen receptor T-cell therapy currently under investigation for patients with relapsed/refractory multiple myeloma (RRMM). The phase Ib/II CARTITUDE-1 trial (NCT03548207) was designed to assess the safety and efficacy of cilta-cel for patients with heavily pre-treated RRMM, and the use of cilta-cel in earlier lines of treatment is being evaluated in the CARTITUDE-2 trial (NCT04133636) of lenalidomide-refractory patients with MM who have received 1–3 prior lines of therapy.
One-year follow-up data from the CARTITUDE-1 trial has previously been reported on the Multiple Myeloma Hub and recently published in Lancet.1 The overall response rate for cilta-cel for patients with RRMM who had received ≥3 prior therapies was 97%, with a stringent complete response rate of 67%, and 12-month progression-free survival and overall survival rates of 77% and 89%, respectively.
The extended 18-month results from CARTITUDE-1 and initial results from CARTITUDE-2 were reported by Saad Usmani2,3 and Mounzer Agha4, respectively, during the 2021 ASCO Annual Meeting and the European Hematology Association (EHA)2021 Virtual Congress. Here we summarize their findings.
CARTITUDE-1 updates2,3
The CARTITUDE-1 trial design, previously described on the Multiple Myeloma Hub, is summarized in Figure 1.
Figure 1. Trial design*
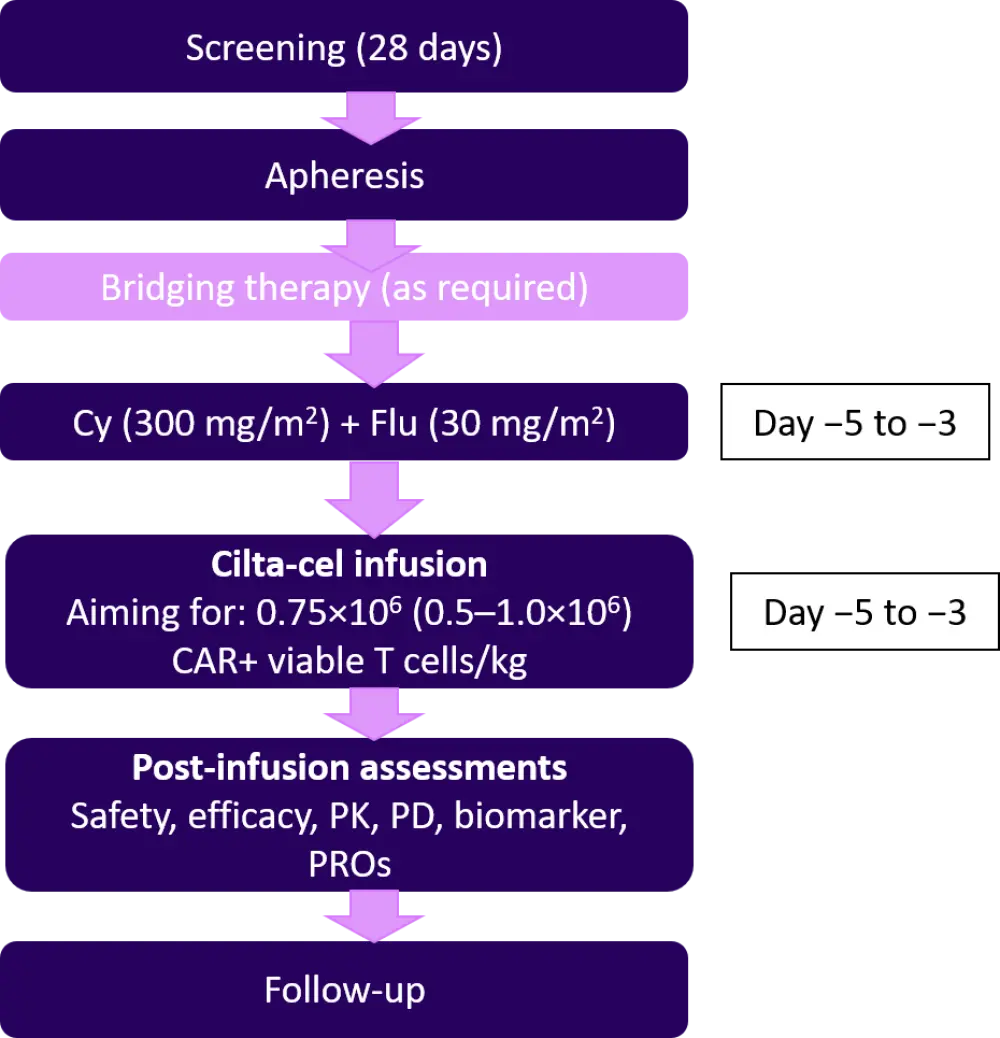
CAR, chimeric antigen receptor; cilta-cel, ciltacabtagene autoleucel; Cy, cyclophosphamide; Flu, fludarabine; PD, pharmacodynamics; PK, pharmacokinetics; PRO, patient-reported outcome.
*Data from Usmani, et al2,3.
Efficacy
Efficacy outcomes after a median follow-up of 18 months (range, 1.5–30.5 months) are summarized in Table 1.
- Responses deepened after the extended follow-up, with an increase in the stringent complete response rate from 67.0% at 12 months to 80.4% at 18 months.
- Response rates were comparable across different subgroups, including number of prior therapy lines, refractoriness, extramedullary plasmacytomas, and cytogenetic risk.
- Almost all evaluable patients were minimal residual disease negative at 10−5 (91.8%).
- For all patients, 18-month progression-free survival and overall survival rates were 66.0% and 80.9%, respectively.
Table 1. Efficacy outcomes*
|
CI, confidence interval; CR, complete response; MRD, minimal residual disease; ORR, overall response rate; OS, overall survival; PFS, progression-free survival; PR, partial response; sCR, stringent CR; VGPR, very good partial response. |
|
|
Outcome |
N = 97 |
|---|---|
|
ORR, % |
97.9 |
|
sCR |
80.4 |
|
VGPR |
14.4 |
|
PR |
3.1 |
|
MRD negativity at 10−5, % |
|
|
All patients/patients with ≥CR |
57.7/43.3 |
|
All MRD evaluable patients†/patients with ≥CR |
91.8/89.4 |
|
18-month PFS, % (95% CI) |
66.0 (54.9–75.0) |
|
Patients with sCR |
75.9 (63.6–84.5) |
|
18-month OS, % (95% CI) |
80.9 (71.4–87.6) |
Safety
No new safety signals were observed with the extended follow-up. Although 94.8% of patients had cytokine release syndrome (CRS), 94.6% of these events were Grade 1 or 2, and resolved within 14 days of onset in 98.9% of patients.
There was no new incidence of neurotoxicity, and no additional movement and neurocognitive treatment-emergent adverse events (TEAEs) were identified. The five patients (5%) with movement and neurocognitive TEAEs had ≥2 of the following risk factors:
- high tumor burden;
- Grade ≥2 CRS;
- immune-effector cell-associated neurotoxicity syndrome (ICANS); and
- high chimeric antigen receptor T cell expansion and persistence.
Patient management strategies have now been successfully implemented in new and ongoing CARTITUDE trials of cilta-cel to prevent or mitigate these TEAEs, including:
- enhanced bridging therapy to reduce tumor burden;
- early and aggressive treatment of CRS and ICANS; and
- handwriting assessments and extended monitoring.
Cilta-cel in earlier lines of therapy: initial results of CARTITUDE-24
Further clinical investigations of cilta-cel include its evaluation for the treatment of lenalidomide-refractory patients with MM after 1–3 prior lines of therapy in the phase II CARTITUDE-2 study. A detailed overview of the trial design and initial results were provided by Mounzer Agha during his interview with the Multiple Myeloma Hub, which can be viewed below.
Initial results of cilta-cel, a CAR T-cell therapy, in earlier lines of treatment
Concerning neurotoxicity, 15% of patients (n = 3) had ICANS, all were either Grade 1 or 2 and resolved upon treatment with steroids. One patient (5%) exhibited Grade 2 isolated facial paralysis, was treated with dexamethasone, and recovered after 51 days. With the implementation of patient management strategies, no patients experienced movement or neurocognitive TEAEs seen in the CARTITUDE-1 trial.
Conclusion
Extended follow-up data from the phase Ib/II CARTITUDE-1 study has shown that cilta-cel has durable efficacy and a manageable safety profile for heavily pre-treated patients with MM. For earlier lines of treatment, initial data from the phase II CARTITUDE-2 trial indicates that cilta-cel promotes early and deep responses, with an overall response rate of 95% and complete response or better in 75% of patients. Toxicity was considered manageable, and with the implementation of patient management strategies there was no incidence of movement or neurocognitive TEAEs in this preliminary analysis.
The phase III CARTITUDE-4 (NCT04181827) trial is now underway to compare the performance of cilta-cel with either daratumumab + pomalidomide + dexamethasone or pomalidomide + bortezomib + dexamethasone for patients with 1–3 prior lines of therapy.
References
Please indicate your level of agreement with the following statements:
The content was clear and easy to understand
The content addressed the learning objectives
The content was relevant to my practice
I will change my clinical practice as a result of this content


 Mounzer Agha
Mounzer Agha